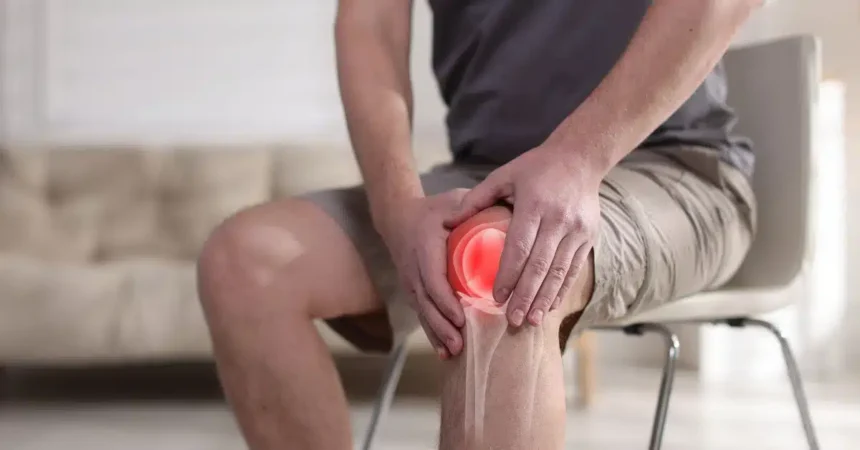
Arthritis is a medical term for inflammation and swelling in one or more joints. The condition affects various parts of the body, but the foot and ankle are frequently impacted because they support the body’s weight. Here is more information on the clinical characteristics of arthritis in the foot, its causes, and the available medical interventions for managing joint pain:
What Is Arthritis?
In podiatry, arthritis refers to the deterioration of cartilage and inflammation of the linings of the foot and ankle joints. The human foot contains many joints, and any of these can be susceptible to the degenerative changes associated with the disease. This degradation leads to direct bone-on-bone contact, which results in pain and limited mobility for the patient.
The condition involves the breakdown of the smooth cartilage that covers the ends of bones. This cartilage functions as a cushion and allows for smooth movement, but its loss compromises joint mechanics. The joint structure may change over time, with bone spurs developing in response to the friction.
What Are the Different Types?
Osteoarthritis is a common form of the condition, and it is often referred to as “wear-and-tear” arthritis. It typically manifests in older adults as cartilage naturally breaks down over decades of use. The disease progresses slowly, with pain and stiffness worsening gradually as the joint surface erodes.
Rheumatoid arthritis is a systemic autoimmune disorder in which the immune system attacks the synovium. The synovium is the lining of the joint, and its inflammation causes fluid buildup and pain. Post-traumatic arthritis develops after an acute injury to the foot or ankle, such as a fracture or severe sprain. This condition operates similarly to osteoarthritis, but the degeneration stems from the initial trauma rather than gradual aging.
What Causes It?
Multiple factors contribute to the onset of arthritis in the lower extremities. Advancing age is a primary determinant, as the body’s ability to repair cartilage diminishes over time. Genetic factors also play a role, with a family history of arthritis increasing the likelihood of a patient developing the condition. Structural abnormalities in the foot, such as flat feet and high arches, can accelerate the development of arthritis.
What Are the Symptoms?
The presentation of arthritis in the foot varies depending on the specific joint affected and the severity of the disease. Pain and tenderness are the primary complaints, and these sensations may intensify during weight-bearing activities such as walking or standing. The pain may subside during rest and return once activity resumes. Swelling and warmth around the joint are common indicators of active inflammation.
What Are the Management Options?
Pharmacological management may begin with nonsteroidal anti-inflammatory drugs (NSAIDs) to control symptoms. For autoimmune conditions like rheumatoid arthritis, immunosuppressant medications are beneficial. These drugs work by inhibiting the immune system’s attack on joint tissues, and this helps prevent further damage. Disease-modifying antirheumatic drugs (DMARDs) preserve joint function and integrity by targeting the underlying disease process rather than just masking symptoms.
When oral medications provide insufficient relief, corticosteroid injections offer a targeted approach. A clinician injects a potent anti-inflammatory medication directly into the affected joint space. This procedure reduces localized inflammation, and it provides relief that can last for several months. Physical therapy helps maintain joint function and reduce pain.
Manage Your Joint Pain Now
Effective management of foot and ankle arthritis requires a comprehensive evaluation and a tailored treatment plan. Early intervention helps preserve joint function, and it minimizes the impact of the condition on daily mobility. Consult a podiatrist to determine the most appropriate course of action for your specific symptoms and condition.